
Delivery of the Baby
During delivery, your baby exits your body, followed by the placenta. In preparation for the delivery, you may be moved into a birthing or delivery room. You may also remain in the same room for both labor and delivery. Your partner is encouraged to be actively involved in the childbirth process by helping you with relaxation methods and breathing exercises.
Positions for delivery may vary, ranging from squatting or sitting positions to semiseated positions. In a semiseated position, you are partially lying down and partially sitting up, allowing gravity to help you push the baby through the birth canal. Your delivery position depends on your preference, the recommendation from your health care provider and the health of your fetus.
During the delivery process, medical personnel will continue monitoring your vital signs, including blood pressure and pulse, and the fetal heart rate. Your health care provider will examine your cervical opening to determine the position of your baby’s head and continue to support and guide you in your efforts to push.
Delivery can be done either vaginally or by C-section.
Vaginal Delivery
During a vaginal delivery, your health care provider will assist the baby’s head and chin out of the vagina when it becomes visible. Once the head is delivered, your health care provider will apply gentle downward traction on the head to deliver the shoulders, followed by the rest of the body. The baby turns itself as the last movement of labor.
In some cases, the vaginal opening does not stretch enough to accommodate the fetus. If the baby is in distress, it may be necessary to accelerate delivery using an episiotomy. During this procedure, the doctor cuts the vaginal wall and the perineum (area between the thighs, extending from the anus to the vaginal opening) to help deliver the baby. Episiotomies are not needed for every delivery and are not performed routinely.
After the delivery of your baby, you will be asked to continue to push during the next few uterine contractions to deliver the placenta. This process may take up to 30 minutes. Once the placenta is delivered, any tear or episiotomy cut is repaired. Your health care provider will likely give you oxytocin to help contract the uterus. This drug will be injected into your muscles or delivered intravenously. The uterus is then massaged to further help it contract and to help prevent excessive bleeding. Some bleeding is normal and should be expected following a vaginal delivery.
Cesarean Section
If you’re unable to deliver your baby vaginally, your baby will be delivered by a C-section. This surgical procedure is usually performed in an operating room or a designated delivery room. Some C-sections are planned and scheduled, while others may be performed as a result of complications that occur during labor.
Once the anesthesia has taken effect, the physician will make a cut in the abdomen and create an opening in the uterus. After the amniotic sac is opened, the baby is delivered through the opening. During the procedure, you may feel some pressure and/or a pulling sensation.
Following the delivery of your baby, your health care provider will stitch up your uterus and the cut that was made in your abdomen. After a C-section, you may still experience some vaginal bleeding.
Conditions for a C-Section
Several conditions may increase your chance of delivering via C-section, including:
- Abnormal delivery presentation
- A previous C-section
- Fetal distress
- Labor that fails to progress or progresses abnormally
- Placental complications, such as placenta previa (the placenta blocks the cervix, which could cause the placenta to prematurely detach from the uterus)
- Twins, triplets and higher-order multiple gestations
Possible Labor and Delivery Complications
Although serious complications are rare during labor, the most common complications include:
Fetal Meconium
When the amniotic sac ruptures, the normal color of the amniotic fluid is clear. If the amniotic fluid is green or brown in color, it may indicate fetal meconium, which is normally passed after birth as the baby’s first bowel movement. Meconium in the amniotic fluid may be associated with fetal distress.
Abnormal Fetal Heart Rate
The fetal heart rate helps indicate how well your baby is handling the contractions. This vital sign is usually monitored electronically during labor. The normal range is between 120 and 160 beats per minute.
If your baby appears to be in distress, your health care provider may take immediate action to stabilize your baby’s heart rate. You may be given oxygen, an increase in intravenous fluids or a new labor position.
Abnormal Fetal Positions During Delivery
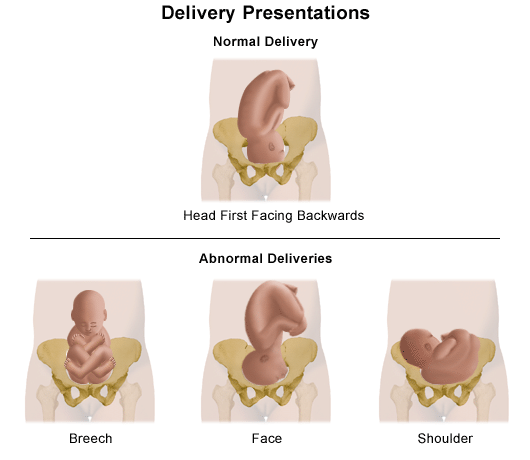
The normal position for your baby during birth is head down, facing your back. If your baby is not in this position, it can make delivery through the birth canal more difficult. The following are the most common abnormal fetal delivery positions:
- Head down but facing your front
- Face down in your pelvis (instead of the top of the fetal head)
- Brow down in your pelvis
- Breech (buttocks or feet are down first in your pelvis)
- A shoulder or arm in your pelvis
Depending on the position, your health care provider may try to deliver the fetus as it presents itself, attempt to turn the fetus before delivery or perform a C-section.


















